This is a plain English summary of an original research article. The views expressed are those of the author(s) and reviewer(s) at the time of publication.
People with a lung condition and severe mental illness can find it difficult to access primary care. Research outlined the barriers faced by people with both of these long-term conditions. It suggested that social prescribing could help overcome some of the problems.
This study included people who had both a severe mental health condition (such as psychosis), and a lung condition that causes breathing difficulties (asthma or chronic obstructive pulmonary disease, for example). It found that people with both conditions could be disabled and isolated.
Participants said that they found it difficult to leave the house to access healthcare, and often relied on friends and family to take them to appointments. Once at a consultation, they found that clinicians used medical jargon, and did not consider how both of their conditions, together, impacted their health and wellbeing.
The study concluded that this group of people need support to navigate the healthcare system. Regular contact with the same clinician was helpful. It recommended that social prescribing could help them build support networks.
Further information on mental health conditions, asthma and chronic obstructive pulmonary disease is available on the NHS website.
What’s the issue?
Severe mental health conditions include psychosis (people may see, hear or believe things that are not real) and bipolar disorder (extreme mood swings). The anxiety, depression and disordered thinking associated with these conditions mean people often struggle to manage their own health. On average, they live 20 years less than others in the general population.
A long-term lung condition adds further challenges. The combination of lung and mental health conditions is common, partly because people with severe mental health conditions are more likely than others to smoke. They are also more likely to live in deprived areas.
People with both severe mental health and lung conditions tend to have poor access to healthcare, and poor outcomes. For example, they are admitted to hospital with breathing issues more often than people without severe mental health conditions.
The NHS has introduced measures to improve healthcare for people with lung conditions. Personalised care plans include support to help people self-manage their condition, such as by quitting smoking. However, there is little research into the experiences of people with both severe mental health and lung conditions.
These researchers interviewed people with both conditions about their experiences in primary care. A wider panel (including researchers and those with lived experience, but also GPs, nurses and charity workers) discussed the interviews and developed recommendations to improve the quality of care.
What’s new?
The study included 16 people who had both a severe mental health and a lung condition. They were aged 45 – 75 years, and were being treated at one of 8 GP practices in South Yorkshire. Most were current or ex-smokers, lived alone, did not have formal qualifications and lived in areas of deprivation.
Researchers asked them about their experience of their conditions and the care they receive.
During the interviews, 3 key themes emerged.
- A lack of social support. People tended to rely heavily on friends and family. Many felt isolated and were either unable or reluctant to leave their own home. Poverty, unemployment, poor access to transport, and the burden of mental health symptoms increased their disability. One said: “When I’m really ill, I can’t leave the house, I can’t leave my bedroom, I can’t go anywhere, I can’t do anything.”
- Challenges of self-managing health. People could struggle to understand medical jargon during consultations and might not fully understand their condition or how to manage it. Many self-managed anxiety by smoking. Community schemes to help people quit smoking did not always accommodate complex psychological needs. One participant said: “I’ve nowt else in my life but smoking… I’ve always been told what to do and what not to do and smoking’s something I choose to do on my own.”
- Difficulty in accessing healthcare. People often did not trust practitioners they did not know. Most found it difficult to navigate the fragmented healthcare system, and often waited until they were very unwell before seeking urgent care. They felt that practitioners did not recognise how their conditions interact, and did not adapt treatment plans accordingly. One interviewee said: “…if I get…restless about asthma and that kicks off like a bit of a panic attack, and then that’s sort of where the bipolar comes in.”
Discussion groups involved 21 people in all (clinicians, charity workers, commissioners, health and social care managers, and people with lived experience).
Potential solutions included:
- continuity of care: seeing the same clinician each time
- helping people to navigate the healthcare system, and ensuring that their experiences inform service design
- social prescribing to help people build up support networks and, for example, helping them get involved in local walking groups or gardening projects.
Why is this important?
This research demonstrates how severe mental health conditions can interact with lung conditions. The combination can make people disabled, isolated, and unable to access quality healthcare.
Friends and family help many people with these conditions access healthcare. Social prescribing could help people build up social networks they can rely upon, as well as improving their physical and mental health.
A key finding was that people with both conditions need a person-centred approach. Treatment plans need to meet the needs of the individual, and they may need help to manage their own health. Many people will need support to get through the healthcare system. Such measures could reduce the need for emergency healthcare.
What’s next?
Social prescribing interventions need to be developed and assessed to see if they improve people’s health. Interventions should help people to build up their support networks, which could in turn help them to access healthcare.
The research team created a visual summary to share with practitioners. It highlights issues raised in the paper.
All but one of the interviewees were White British. Cultural barriers to discussing mental health may have discouraged people from other ethnic groups, along with the lack of interpreter support for non-English speakers. Further studies are therefore needed to see if the findings apply to other ethnic groups.
Materials for participants must be clear and simple, to enable people with lower health literacy to take part in research. The researchers say this population is often the most underserved.
The study was conducted in South Yorkshire. Further work should assess whether these findings apply elsewhere in the UK.
You may be interested to read
This summary is based on: Mitchell C, and others. Primary care for people with severe mental illness and comorbid obstructive airways disease: a qualitative study of patient perspectives with integrated stakeholder feedback. BMJ Open 2022;2:e057143
Lived experience of people with mental and physical health conditions: Coventry P, and others. Living with complexity; marshalling resources: a systematic review and qualitative meta-synthesis of lived experience of mental and physical multimorbidity. BMC Family Practice 2015;16:171
Information about many mental health conditions is available from the charity Mind
Asthma and Lung UK has further advice about managing anxiety and asthma and managing COPD (chronic obstructive pulmonary disease).
Infographic credit and permissions: NIHR Evidence has permission to feature the visual summary above, which was created by Nifty Fox Creative and commissioned and funded by the grant.
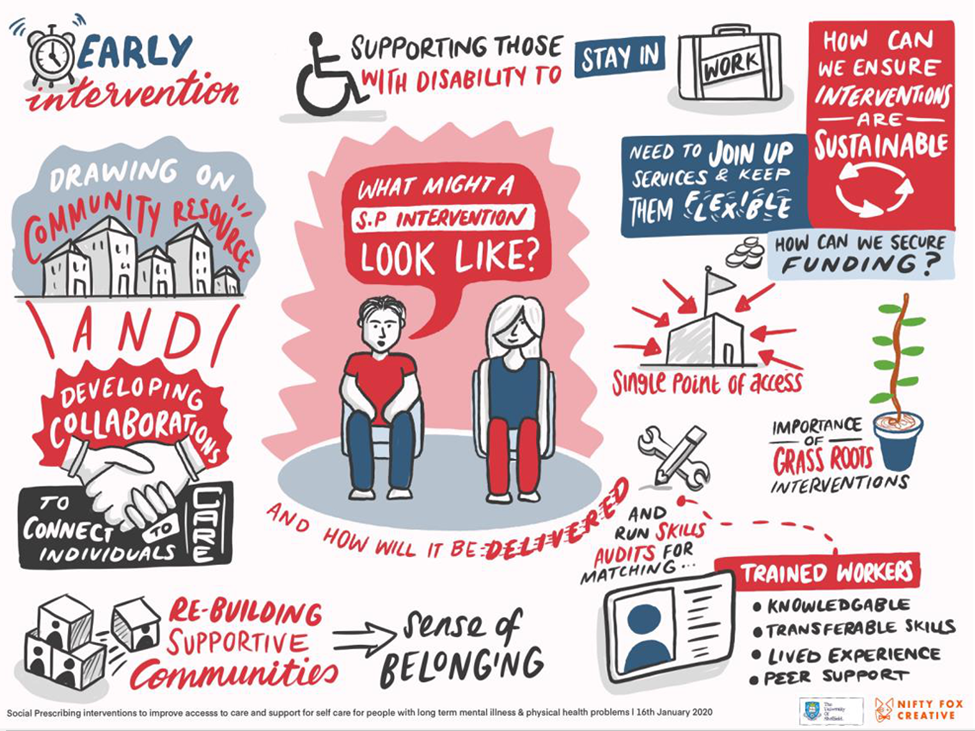
Infographic descriptive text: The infographic describes social prescribing interventions and the steps needed to deliver them. It outlines the need:
- for early intervention
- to draw on community resources to develop partnerships within the care sector
- to rebuild support networks through local projects, and to create a sense of belonging
- to support people with disabilities to remain in work
- to make services flexible to meet people’s personal needs
- to secure funding for social prescribing interventions
- to train individuals to support this group of people.
Funding: This research was part-funded by the NIHR CLAHRC Yorkshire and Humber, an NIHR RCF grant from Sheffield and Social Care NHS Trust and a small grant from the Clare Wand Charitable Fund (BMA).
Conflicts of Interest: The study authors declare no conflicts of interest.
Disclaimer: Summaries on NIHR Evidence are not a substitute for professional medical advice. They provide information about research which is funded or supported by the NIHR. Please note that the views expressed are those of the author(s) and reviewer(s) at the time of publication. They do not necessarily reflect the views of the NHS, the NIHR or the Department of Health and Social Care.
NIHR Evidence is covered by the creative commons, CC-BY licence. Written content and infographics may be freely reproduced provided that suitable acknowledgement is made. Note, this licence excludes comments and images made by third parties, audiovisual content, and linked content on other websites.