How can local authorities reduce obesity?
Insights from NIHR research
‘Obesity is considered to be one of the most serious public health challenges of the 21st century. It is having an impact on people’s lives now, across the generations, in terms of our quality of life, our risk of developing chronic diseases such as type 2 diabetes and its association with common mental health disorders. Doing nothing is not an option. Without action, the health of individuals will continue to suffer, health inequalities associated with obesity will remain and the economic and social costs will increase to unsustainable levels’ (Local Government Association).
The NIHR invests more than £1bn a year in research to improve the health and wellbeing of the nation. Over the last decade, we have invested heavily in research aimed at preventing or managing obesity. We want to support good local decision making by ensuring that investment decisions can be based on sound evidence. This will maximise the impact of stretched local resources.
This Themed Review identified 143 NIHR-funded studies on obesity that are relevant to local authorities. An array of interventions, settings, and study types were considered; some of the research is in emerging fields. Ongoing research that the NIHR funded recently is highlighted, since upcoming results could help address gaps in the current evidence base.
The Review drew on the expertise of a group of practitioners, researchers and members of the public. Conversations with a range of local authority staff and other key stakeholders gave us valuable insights. They helped us draw the research together in a meaningful way, put it in context and made sure the Review addressed key questions.
The interventions covered by NIHR research were specific to local contexts and may not always be applicable elsewhere. For example, local councils told us that certain food advertising restrictions on the London Underground, which demonstrated impact in London, would be harder to achieve in their local context. In addition, studies generally ran for 12 months or less; some interventions could take much longer to show an impact.
This Review covers 143 NIHR-funded studies, of which 32 were underway when the Review was completed. The chart below shows how many studies were funded across different areas of obesity research.
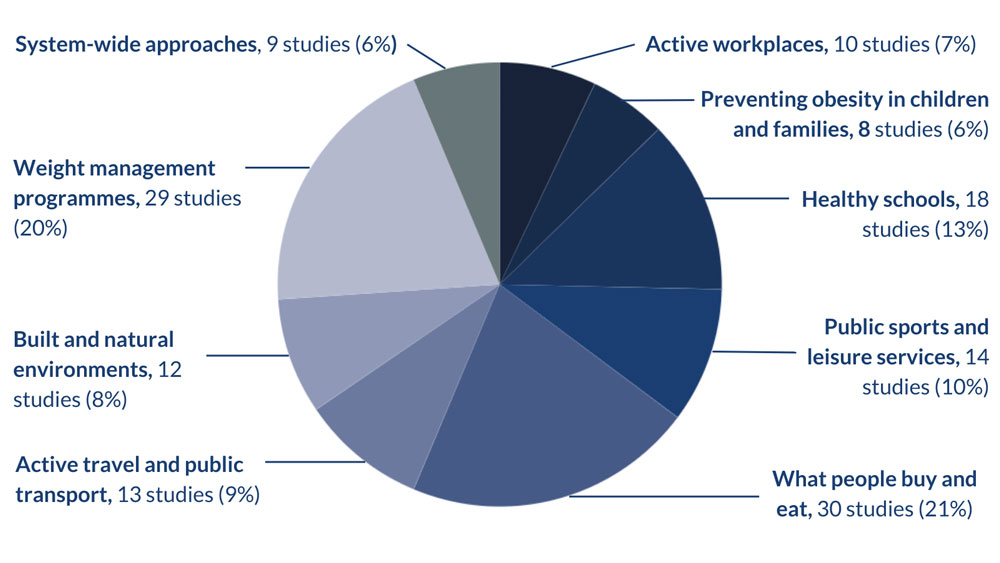
You can find a table version of the data contained in this chart here.
Context
Obesity is a major health crisis in the UK (Department of Health and Social Care) and more than a quarter of adults are living with the condition.
Obesity in the UK
A text alternative for this graphic and the references used to produce this graphic can be found here.
Consuming more calories than are needed leads to weight gain. Boys living with obesity or overweight, for example, have been found to consume between 140-500 excess calories each day (UK Health Security Agency). Globally, there has been an increased intake of energy-dense foods that are high in fat and sugars (World Health Organisation), and UK consumers generally do not meet the standards recommended for a healthy diet (Rand). However, many factors drive obesity; there is no single dominant cause.
Early life experiences – including growth patterns in the first weeks or months of life – affect the risk of obesity years later (Foresight). Children of parents living with obesity are more likely to develop obesity themselves. And by the end of primary school, 35% of children are living with overweight or obesity (UK Parliament).
The NHS spent an estimated £6.1 billion on overweight and obesity-related ill-health in 2014 to 2015 and these costs are expected to reach £9.7 billion by 2050 (Public Health England). The costs to the wider economy include higher levels of sickness and absence from work, and have been predicted to reach £49.9 billion per year by 2050 (Foresight).
Local authorities face a mass of competing pressures. They have to respond to rising care needs, tackle health inequalities, and reach net zero. They have to maximise childrens’ life chances and build back local economies after the pandemic. Obesity has an impact on many of these priorities. It drives up care needs, has an adverse impact on life chances and reduces economic productivity. By contrast, strategies to reduce obesity can have a positive impact on the environment and progress towards net zero. For example, more active travel, by foot or bicycle, can also reduce road traffic.
The COVID-19 pandemic has brought the obesity crisis into sharp relief. People living with obesity have an increased risk of severe illness and death from COVID-19 (Public Health England). The pandemic has also widened the health inequalities associated with race, gender and where we live (Local Government Association). Children living in the most deprived areas in England are more than twice as likely to live with obesity than those living in the least deprived (NHS Digital). People living in the most deprived areas are less likely to meet ‘5 a day’ guidelines for fruit and vegetable intake, or to meet physical activity guidelines (Department of Health and Social Care); young people from the least affluent families tend to be the least active (Sport England). Eating a healthy diet relies on people having consistent access to nutritious food (food security). In the UK, food and non-alcoholic drink is the fourth largest household expense (Department for Environment Food and Rural Affairs). When household income is stretched, choice of food is likely to be limited by its cost, and the ability to eat a healthy diet is threatened. Tackling obesity therefore goes hand in hand with the levelling up agenda. In its response to this agenda, the Local Government Association stresses the need to reduce poor health outcomes (including obesity) as well as economic imbalances between regions (Local Government Association).
The need for a whole systems approach to tackle obesity – comprising national policy, multinational actions on food and retail, together with local initiatives – is increasingly recognised. Local authorities can directly support aspects of this approach (Public Health England). At a local level, a systems approach moves away from a series of isolated interventions. Instead, it seeks to understand the system as a whole, and the interventions that represent powerful levers for change. Stakeholders from across the local systems need to collaborate for this approach to be possible. Activities where a council can take action need to be identified (for example, natural spaces, travel infrastructure, or the local food environment). And systems thinking, which can help make sense of a complex situation by looking at the relationships between different parts (rather than considering each separately) will be needed to generate dynamic and flexible interventions (Local Government Association).
Some NIHR funded research seeks to alter people’s behaviour directly (e.g. through education to promote a healthy diet). Other projects adapt the environments in which we live, work and play to support people to be active and eat healthily. The research may be for people living with obesity, or may aim to prevent obesity in the broader population. Several interventions aim to increase physical activity. However, the link between increased activity and obesity is not clear cut. Physical activity on its own is unlikely to prevent obesity, but, as part of a wider package of initiatives, can help achieve change. Most research to date has evaluated specific, single interventions, and there has been less on combinations of interventions that address multiple aspects of the system.
In this Review, we cover areas in which local authorities can take action:
- Influencing what people buy and eat
- Encouraging healthy schools
- Expanding access to public sports and leisure services
- Promoting active workplaces
Providing weight-management programmes - Designing built and natural environments
- Enabling active travel and public transport
- Preventing obesity in children and families
- Embracing system-wide approaches
We draw conclusions to help local authorities make sense of the research, and use it to inform decision-making.
Conclusions and key actions
Obesity is the result of interplay between many factors (Foresight). The context in which local authorities operate – levels of deprivation, resources, urban and rural geography, and other competing priorities locally – influences the approaches that can be taken to prevent obesity. National initiatives, such as taxes or other regulatory changes, are important. Supporting people to maintain a healthy weight requires action on many levels: individual, organisational, across whole systems, local and national.
This review draws on the breadth of NIHR research relevant to obesity, conversations with staff at local councils and at national organisations, as well as feedback from a group of practitioners, researchers and members of the public. Together they have helped us identify evidence-based actions that local authorities, working with their local partners, can take to reduce obesity in their communities.
Investing in active travel, infrastructure, community sport and physical activity
Investing in active travel and increasing access to public transport should be key elements of a systems-wide strategy that aligns with local sustainability and carbon reduction plans. Active travel can encourage people to become more physically active. It has been shown to lower BMI in children, to reduce health inequalities and to provide value for money. Research points to good practice. For example, where walking and cycling paths connect with transport hubs, they are more likely to be used. Encouraging use of public transport can have health benefits for certain groups of the population and goes hand in hand with active travel. Further research is needed to clarify which groups engage with active travel and how it addresses health inequalities.
Changes to the built environment, including access to green spaces, can increase physical activity and improve environmental sustainability. Environments that encourage walking and are close to natural spaces can increase physical activity and have been associated with a lower BMI in children. Investing in environmental design that supports active lifestyles is in line with environmental imperatives. Multiple factors underpin how people use these spaces. Staff at local councils emphasised that some residents rarely leave their locality and therefore will only access green and blue spaces that are in close proximity. Small changes can encourage use of parks, such as removing bushes that obscure the line of sight and can make park users feel unsafe.
Free access to public sport and leisure services can help people to be more physically active, but the picture is mixed over its effectiveness, and whether it reaches those most in need. Programmes to encourage walking can be cost-effective, but findings on community exercise programmes are mixed – studies have not demonstrated sustained physical activity beyond 12 months. The effectiveness of programmes depends on the local area served, the level of deprivation, and the extent of inactivity. The evidence is mixed on whether extending access to public gym and swim facilities reaches those living in disadvantaged neighbourhoods. This will be more relevant for some places than others. Travel to public facilities can also be a key consideration. Behavioural change techniques may be needed to encourage people to use public sport and leisure services; research is needed to find out. In the meantime, local authorities may decide to prioritise investment in infrastructure, the environment and active travel, over public sport and leisure services. Or they may decide that a wider range of solutions is needed that closer align to tackling health inequalities.
Influencing behaviour from childhood
Programmes aimed at preventing obesity in children and young people in the community can be effective, but the impact varies across age groups. Few interventions over the last 25 years have targeted the wider determinants of childhood obesity (such as infrastructure, environmental and policy factors). Instead, they have encouraged children to change their individual food and activity behaviours. Cuts to Sure Start children’s centres had an adverse effect on obesity in young children. There are different services in Northern Ireland, Scotland and Wales and the impact of cuts on similar services may vary according to the local context. There is evidence that interventions that include diet or physical activity components, or both, can reduce the risk of obesity in children aged 0 to 12 years and do not worsen health inequalities. However, most studies have reported outcomes at 12 months or earlier, so the long-term effectiveness of these interventions is not known. Young teenagers in particular need approaches that chime with their interests and the importance of friendship groups.
Interventions in schools to increase physical fitness or alter dietary habits have achieved limited results; most NIHR-funded interventions in UK schools have not been effective. Research tells us that leadership and parental and community involvement are likely to support health promotion in schools. Local authority staff emphasised the importance of ‘whole school’ approaches with a wide focus on health promotion beyond just maintaining a healthy weight. Local authorities may consider that attention should be redirected away from interventions focused on changing the behaviours of school children (particularly of primary school age). Instead, they could concentrate on the wider environmental factors that influence behaviour through the lifecourse.
Supporting people living with obesity
Weight management programmes for people living with overweight or obesity are part of a broader strategy to tackle obesity. Research has shown these programmes may be effective for short-term weight loss. The key question is how long weight loss can be sustained; investing in targeted support to maintain weight loss after a programme has ended has not been shown to be effective. Factors associated with success include: group-based programmes over one-to-one interventions; tailored programmes; and running weight management programmes for children in school settings where attendance is mandatory. More research is needed on the most effective components of weight management programmes. Local authorities told us they are investing in family-based weight management programmes – which have achieved mixed results in NIHR-funded research to date. Barriers found in previous interventions include the costs of participation to families, and sustaining engagement. Addressing these and other barriers could improve the success of programmes.
Strategies that reflect societal shifts, e.g. in the workplace
Local authorities are expected by NICE to be exemplars of workplaces that prevent and manage obesity; however with a move to hybrid working, local authorities may want to direct attention away from office-based workers. NIHR research provided limited support for actions to encourage office workers (including in local councils) to sit less and move more. Local authorities may decide that attention is better directed at creating environments that support active behaviours and reduce calorie consumption across a range of settings, and in incentivising everyone to be active throughout the working day.
Reducing excess calorie consumption
Local authorities can take action on the food environment; targeting out of home foods and restricting advertising of high fat, salt and sugar products could reduce excess calorie consumption. Working with food outlets to reformulate recipes and portion sizes, reflecting a ‘health by stealth’ approach, has been well-received by outlets and customers. Further research is needed into how these interventions impact consumption, overall diet, and body weight. Restricting junk food advertising can impact household food purchasing decisions. However, local authorities’ powers to influence advertising vary; decisions to restrict advertising may need to be squared with the loss of lucrative advertising revenue, highlighted by some local council staff. People’s agency and ability to make choices (for example, to eat healthily versus heat their homes), or their dependence on food banks or food pantries, dictate the success of strategies to alter the food environment, local council staff said. Planning guidance to restrict new fast-food outlets near secondary schools has not, as yet, been shown by NIHR research to be effective in decreasing the number of outlets. However, this was possibly due to low numbers of new outlets opening during the study; long term monitoring of exclusion zones around schools are needed. The rise of home food delivery services poses challenges to influencing the food environment, at the same time as allowing new business models to flourish.
Local actions to support system-wide approaches
More research is needed to assess local authority actions as part of whole system approaches to obesity. The whole system is about bringing together transport planning and spatial planning decisions, education departments, parks and greenspace departments, leisures services, the NHS, integrated care systems, food retailers and more, to work together to reduce obesity. Directors of Public Health have a responsibility to lead a whole system approach to the public’s health across the public sector, within local authorities, and across the NHS and other sectors and agencies, to facilitate system-wide change (Department of Health and Social Care). The research covered by this review has looked at just some of the levers that local authorities can use as part of system approaches. It also highlights some of the enablers and barriers to implementing multi-pronged combinations of interventions, including the importance of leadership, community engagement and having sufficient time and resources to allow initiatives to take effect and demonstrate impact.
The NIHR is continuing to fund research relevant to this agenda. Local authorities can get in touch with NIHR with proposals for research projects, to get support evaluating interventions already in place, or to submit a research suggestion where they have identified a need for more research to help with evidence-based decision making.
Foreword
Commentaries
“Obesity is a complex problem with a large number of different but often interlinked causes. No single measure is likely to be effective on its own in tackling obesity. To have a significant impact on obesity levels, it is clear that everybody needs to get involved. Local authorities are particularly well placed as the functions they are responsible for serve all generations in society and can directly influence people’s health. This research provides really useful information to support local authorities with implementing a whole systems and whole council approach to address obesity and promote a healthy weight.”
“Obesity prevention continues to be a major public health priority. Recognising that local authorities are uniquely positioned to work with partners and influence the local drivers of obesity, public health teams have been asked to take a whole systems approach. This themed review presents local authorities with a collation of key research findings for interventions targeting individual drivers of obesity. Going forward a step change is needed to look at interventions as part of a system and not in isolation. To support a whole systems approach and build the evidence-base, future research should consider how interventions interact with the context (a complex dynamic system) and consider how they change the system to address obesity.”
“This summary is a good starting point if you want to explore obesity research. If digging deeper, consider not just what does and doesn’t work but the ‘why’ and ‘how’. This is not an overall guide of what to do, for three reasons. First, this review only covers NIHR-funded research. Second, and more broadly, much of the research is inconclusive. For instance, it might say an intervention didn’t work, but not whether it would have worked if it was implemented slightly differently. Finally, the research that has been carried out to date does not represent all topics and types of research evenly (e.g. there is more on individuals than systems).
There is currently no definitive prescription for a multifaceted local authority approach. What does seem to be clear is that local authority action needs to take account of the ‘whole system’ and how it works (in particular the food industry), even if the local authority can only influence a part of it. This is particularly important in the food industry. Local authorities can use their own data and experience and data to help shape and contribute to future research.”
“Obesity is a complex public health challenge. Drawing on complex adaptive systems has enabled detailed descriptions of the determinants of obesity and their interactions. Views differ on what whole systems approaches to tackling obesity mean but the scope of such systems extend beyond single entities. There is a risk that ‘whole systems’ is understood to imply ‘multiple concurrent interventions at various levels and across the entire life course’. This is neither achievable, even with additional resources, nor sufficiently cognisant of the role of simple rules (small changes) in a complex system in producing transformational impact. Future research has to further our understanding of those small changes in sufficient practical detail if we are to achieve sustained impact in terms of a left-ward shift of the dial on the population’s weighing scale. This review is a real welcome step in the right direction but it signals the need for more work.”
“Health & Wellbeing Boards have (since the Health & Social Care Act 2012) been the formal committee of a local authority charged with promoting greater integration and partnership between bodies from the NHS, public health, the voluntary sector and local government. With the introduction of Integrated Care Systems (ICSs) as part of the 2022 Health & Care Bill, system-wide approaches between local health, local authority and voluntary and community sector partners will also be in the remit of integrated care partnerships both at ICS (sub-regional) level and more local Place-based partnership level (at the level of a single unitary authority).
With Place-based Committees and Health & Wellbeing Boards being guided to try and adopt Shared Outcomes in the Integration and innovation White Paper, the opportunity to embrace, develop, plan and implement system-wide approaches for tackling obesity and promoting healthy weight, healthy eating and physical activity throughout the life course has never been greater, nor the need more sharply focussed in both the health and care arena, at both hospital, secondary-care, primary care, community, school and neighbourhood levels. Nor could the need for evidence-led actions be greater, to inform best-practice approaches and evidence-led programmes that have been shown to work as practical interventions.”
Related Content
- Alert | Preventing childhood obesity requires a shift in focus away from individual behaviours towards the wider environment
- Alert | Better pathways promote physical activity and can decrease health inequalities
- Alert | People in the most deprived groups were least likely to take part in the exercise referral scheme, study finds
- Alert | Digital games, apps and e-therapy show promise for helping children manage obesity, anxiety and other long-term conditions
- Alert | Working in groups with ongoing support is valued by people with severe obesity trying to lose weight
- Alert | Diet and physical activity interventions targeting children and youth have different, yet small, effects on preventing obesity
- Alert | Schoolchildren who switch to walking or cycling may have a healthier body weight
- Alert | Cycling to work lowers risk of illness and death compared to driving
- Themed review | Moving Matters – Interventions To Increase Physical Activity
- Alert | Most patients welcome advice from GPs on changing their behaviour to improve health













I am delighted that this Themed Review has been undertaken. The NIHR is a well-oiled machine for commissioning research, but we sometimes lack the time and space to stand back and understand what we have learned from our various outputs. Over time, obesity research has of course encompassed diet and nutrition as well as wider interventions related to travel, the environment and physical activity. It’s a good time to step back and ask what we have learned from this body of research.
Inevitably this review is a snapshot and only part of the vast amount of evidence on obesity. However, it provides us with important pointers about where to go next. At the NIHR, we will continue dialogue with the research and policy communities to make sure that future research targets the areas likely to offer the most value in tackling this complex public health issue. Just as there is no single magic bullet to intervene in obesity, there will be no single path for research. Future approaches will need to complement other research initiatives and activities both within and outside of the NIHR.
Professor Brian Ferguson, Programme Director NIHR Public Health Research (PHR) Programme