Please note that this summary was posted more than 5 years ago. More recent research findings may have been published.
Dementia is a group of symptoms associated with a loss of brain function. The symptoms can include loss of memory, mood changes and confusion. There are many different causes of dementia, and many different types, including Alzheimer's disease and vascular dementia. In the UK, 850,000 people currently live with dementia. Around one in 14 people aged over 65 have a form of dementia, and one in six people over 80. The total cost of care is £34.7 billion.
With 52% of the UK public knowing someone who has been diagnosed with a form of dementia, the impact and challenges that this syndrome presents is a major issue of interest and concern for individual patients, families, carers and health services.
This Collection brings together NIHR research relating to dementia. We asked a number of healthcare professionals, carers and service users to comment on selected Alerts that are relevant and important to them. Their commentary provides a valuable insight and highlights what we can learn from the research summarised in the Alerts.
The Alerts included in this collection are:
- Informal dementia carers had to make difficult decisions about paid care during COVID-19
- People with dementia from ethnic minority backgrounds face extra barriers in accessing care
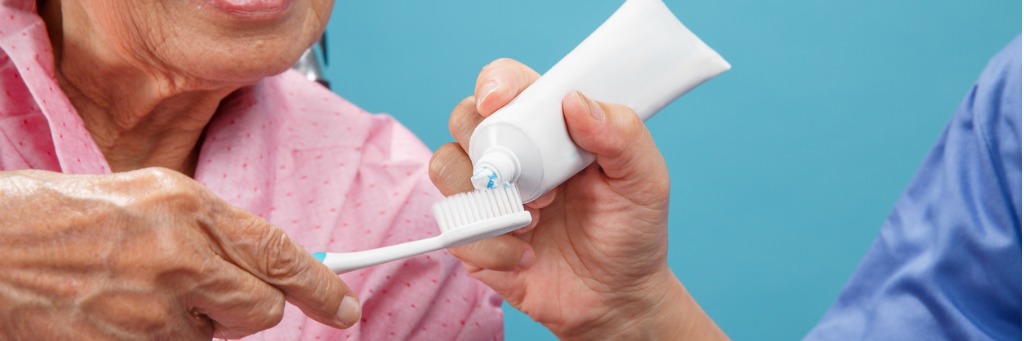
- Careful phrasing of requests by hospital staff could help people with dementia accept care
- Loneliness in people with dementia is linked to social isolation and depression
- People with mild memory problems are left in limbo between health and dementia, and need help to make lifestyle changes
- Most people caring for relatives with dementia experience loneliness
- Occupational therapy at home may benefit people with dementia and their carers
- Working may improve quality of life for carers of people with dementia
- Loneliness, but not social isolation, predicts development of dementia in older people
- Training programme to improve communication between staff and patients with dementia in hospital shows promise
- A less healthy lifestyle increases the risk of dementia
- Goal-setting can help people with early-stage dementia improve function
- Dementia Care Mapping: Care home managers and staff need more support to improve care
Informal dementia carers had to make difficult decisions about paid care during COVID-19
Read the Alert on informal dementia carers
Dr Penny Rapaport - Clinical Psychologist
“What is striking about this research, and will resonate with many reading the summary, is the pace at which family carers and those affected by dementia were having to make potentially life changing decisions early in the pandemic. The family carers interviewed had to take on additional caring responsibilities, which they may not have been equipped for, facing practical and emotional challenges without the usual support mechanisms in place. Many of the concerns raised by the carers seem to relate to existing limitations in home care provision for people living with dementia and the under resourcing of social care more broadly, with the pandemic lockdown bringing these issues into focus. This study therefore has implications beyond understanding the impact of Covid-19, highlighting the need to understand what good quality home care for people living with dementia looks like and the need to invest in social care. These findings also made me curious about the experiences of home care workers who have continued to deliver care to people living with dementia during this period, how they have been supported and protected and the need for further research considering their unique perspectives.”
Peter Green - Former carer
“The close relative I cared for was in precisely this situation described in this study. She had paid carers coming into her home twice every day, as well as the voluntary care from myself and other family members. It was a great worry to the family, because we could not see how we could provide the level of care needed if the paid carers were unable to continue. At that time the availability of personal protective equipment (PPE) was a major concern.
“Myself and another family member had to continue to do all shopping because home deliveries were simply not available to us. Fortunately the care company were very helpful. They reduced the number of different carers entering her house, but PPE was the bare minimum due to the lack of supplies. The improved continuity of care this resulted in was an unexpected benefit. The cost of that care increased because of the additional precautions they had to take. The increased cost of care would, I am sure, be a big factor in many carers' decision making. What is not clear is how the improved guidelines and support would be distributed to unpaid carers.”
Ann Pascoe - Carer
“I really resonated with this Alert and believe the researchers got it spot on. I am a carer for my husband, Andrew, who was diagnosed with vascular dementia in 2006. In the second week of March 2020 I made the decision that no one would come into our house. In the summer, with the relaxation of lockdown rules, I had some people help with activities for Andrew but it all happened outside. Now with winter being back, all the onus is on me to provide full care. Prior to Covid-19 and lockdown I was able to arrange stuff for Andrew while I was away so he was seeing other people and doing other things. My decision to not let people in our house means that the additional support is no longer an option.
“As chair for Connecting Communities in Helmsdale I also understand the situation of support workers who used to go into homes to help with care. Our staff were as frightened to go into people’s homes as people at home were frightened to have them in. Lack of personal protective equipment or knowledge of how to use the equipment along with the fear of contracting Covid-19 contributed to this. With lockdown, we stopped people going in but we have become acutely aware of the mental health and loneliness issues that all of our older folk – one in three people are 65+ in remote, rural Sutherland - are experiencing and we are trying to address this.”
People with dementia from ethnic minority backgrounds face extra barriers in accessing care
Read the Alert the barriers in accessing care
Mohammed Akhlak Rauf - Founder & Director of Meri Yaadain CiC
“I welcome this research and hope it encourages further research in a much needed area of understanding. The first point to add is that the term ethnic backgrounds should be seen as problematic on its own. Everyone is of an ethnic minority or ethnic majority background. Each of the two has a variety of ethnic backgrounds within them, so it becomes difficult to generalise. Having said that, it is imperative that research on Black, Asian, and minority ethnic (BAME) communities is inclusive of the diversity within these communities. Accessing care for minority ethnic people whether living with or caring for someone living with dementia begins with awareness and understanding of dementia. Assessments are still (broadly) not culturally appropriate, services are not culturally competent and post diagnostic support is patchy, particularly where practitioners feel 'they [BAME]’ look after their own.
“BAME carers are often coping with multi-morbidity as well as dementia in a relative. Depression for the person living with dementia as well as the carer creates a double jeopardy, where there are huge gaps in the understanding of social behaviours, yet alone how best to provide adequate support. Language is often cited as a barrier, but our experience tells us that BAME communities themselves are going through a transition – language, values, education, influence of faith, gender roles, expectations, etc. Further research with participants who feel valued – recruitment often requiring trust before participation – will result in data and recommendations which are more meaningful and have a greater impact.”
Isobel Chick - Speech and Language Therapist
“Ethnicity constitutes a barrier to effective care. Adults from ethnic minorities are more likely to be prescribed four or more medications than White British adults, even though multiple medications are known to increase the risk of poor outcomes for people with dementia, such as repeated falls and hospitalisation. People from ethnic minorities are also under-represented in dementia research in general, even though they are more likely to be diagnosed with dementia than the White British population. Further research is needed to explore the reasons behind this, but what is clear is that the health system is not currently meeting the needs of adults with dementia from ethnic minority populations and programmes to engage these communities are not fully successful.”
Careful phrasing of requests by hospital staff could help people with dementia accept care
Read the Alert on phrasing requests
Wendy Mitchell - Diagnosed with young onset dementia in 2014
“This is such a useful and rarely studied issue but the psychological effect of words and body language should never be underestimated by any healthcare professional. We are, after all, in an alien environment. Our routine has disappeared and our comfort setting has disappeared only to be replaced by strange unfamiliar people insisting we drink, eat and take medication. Suspicion as being told would result in refusal so it’s so refreshing to hear of work being done to promote respect by asking, not telling and by suggesting and including the person with dementia in the act. Our refusal would probably lead to a labelling of being a difficult patient, when in fact our refusal may simply be out of confusion or fear.
“So often research sits on the shelf so it’s good to hear that this research had led to a training programme aimed at changing the behaviour and understanding of healthcare staff.”
Sue Hilsdon - Carer and retired occupational therapist
“Taking away doubt in a conversation is vital. Talking in phrases that encourage, persuade, and give positive direction are essential. Approaching a person with dementia, in an insightful, knowledgeable way, will also engender a positive response in almost all situations. Breaking a task down into simple, familiar steps are indeed helpful too. I fully concur with the content of this study.”
Emma Williams - Behaviour Analyst
“This research presented an interesting approach to communication about tasks which are required to be carried out. It can be challenging to engage people with dementia during tasks which may seem aversive or confusing to them (such as during personal care). This research provided a variety of approaches which may increase opportunities for engagement and interaction, although further research is required in other settings. Positive reinforcement should be given to the person with dementia to encourage future interactions and engagement with the tasks. It is important that the needs and wishes of the individual is kept forefront, to provide person-centred care at all times.”
Dr Penny Rapaport - Clinical Psychologist
“At a time when many of those with dementia in hospital cannot have family members visit or advocate on their behalf, and when hospital staff are themselves working under additional pressures and Covid-19 restrictions, this research feels incredibly useful and potentially beneficial for so many. What struck me about this research, as a clinician and a researcher, is that using such in depth observational methods has resulted in very clear and specific evidence as to what good and clear communication looks like. It is for example interesting, that taking a more tentative approach can communicate uncertainty and although as health care professionals we may be trained to communicate in this way in lots of situations, it may be confusing for people living with dementia, especially in an unfamiliar setting like a hospital ward.
“In my own experience, training interventions in dementia care may be limited by not addressing the real-life complexity faced by staff and by it not being possible to build learning into routine, day-to-day care. Having training based on these detailed observations will directly overcome this and highlight to those receiving training that small changes can make a big difference to the lives of people living with dementia in hospital.”
Loneliness in people with dementia is linked to social isolation and depression
Read the Alert on loneliness in people with dementia
Ann Pascoe - Carer
“After reading this Alert, I asked Andrew the question: ‘Are you lonely?’ He responded saying ‘No, I have lots of things to do: I have my radio to listen to; I can watch cricket on the telly; and I’ve got you to talk to.’ This is of course true but the onus gets put on the carer then to provide those activities, their time to talk and to do all the things that the person with dementia wants to do. I believe that loneliness can therefore be dementia-specific, which is contrary to what the Alert highlights. If Andrew didn’t have dementia, I wouldn’t have to plan out his day and spend that extra time as a carer rather than a wife. So I think loneliness in people with dementia is indeed linked to social isolation and depression if they are on their own or if the carer – or someone - isn’t there to help them to do things.
“The Alert also highlights that focussed interventions to identify and tackle loneliness could increase the wellbeing of people with dementia – this is absolutely true. Before lockdown, Andrew used to go to the community centre three times a week and get involved in the Men’s shed and other activities such as art, games and gardening. As a result of lockdown, I have had to bring the ‘community’ to him providing those activities at home. Interestingly, Andrew’s wellbeing and health have not suffered due to the pandemic. He has had no transient ischemic attacks since the start of lockdown. Our doctor believes that this is as a result of me always being with Andrew which makes him feel safe. This again, however, puts the onus on the carer.”
Kathryn Walker - Clinical Research Nurse
“Loneliness and social isolation are a huge issue in the ageing population; particularly in the current climate of Covid restrictions. It is encouraging that this study shows little difference in the occurrence of reported loneliness between the cohort with mild to moderate dementia compared to the general ageing population, however 30–35% of people in both groups reporting loneliness is still alarming. Loneliness, particularly in the ageing population, is linked to a number of conditions such as depression, cognitive decline and poor wellbeing. As well as being distressing for the individual, the resulting impact to the health of these individuals can affect their quality of life and may increase the need for further provision of both health and social care.”
People with mild memory problems are left in limbo between health and dementia, and need help to make lifestyle changes
Read the Alert on mild memory problems
Dr Tom Russ - Consultant Psychiatrist
“This is a very timely and important study – particularly since it is speaking directly to the people concerned to gather their views. There remains substantial uncertainty around people who have some memory changes which aren't too bad who also remain mostly independent in day-to-day activities. Clinicians do not yet have any good tests to predict who in this group will progress and develop dementia (approximately one in nine people each year) and who will not (eight out of nine people). This conceptual uncertainty leads directly to the feeling of being in limbo experienced by people told that they do not have dementia but are not 'normal.’”
Peter Green - Former carer
“This is a very welcome study. A near relative was diagnosed with Alzheimer's disease over a year ago. Following his diagnosis the support services in his area for him and his wife have been excellent. This contrasts greatly to the situation prior to his diagnosis, when it was evident to him and his wife that he was having memory problems. This was a gradual process, worsening over two years. At this time they had no support whatsoever, and they felt this was not helped by the standard ‘memory tests’ used by his GP, which failed to identify any problem. This study is highly relevant to the situation they were in and I am sure would benefit very many people. It should be of interest to healthcare professionals and those in the dementia voluntary sector. Healthcare professionals should take account of patients' own feelings of memory problems and be encouraged to help them to engage with support services.”
Kathryn Walker - Clinical Research Nurse
“Feelings of anxiety and distress are common for this patient group and their families due to the symptoms they experience and the uncertain future they potentially face. The facts presented state that about half of over 65s experience memory problems, with one-fifth having symptoms of mild cognitive impairment. With our ever increasing ageing population, the number of people affected is likely to increase with a larger amount of the UK population being affected. It is important that this patient group receive the support they need to help combat cognitive decline. If the randomised control trial mentioned in the paper is successful, the APPLE-Tree programme that these researchers have developed for this patient group will be a valuable resource to help fight back against the onset of dementia.”
Isobel Chick - Speech and Language therapist
“Specialist support to reduce the risk of developing dementia is vital as the population ages. Adults with mild cognitive impairment require support to make lifestyle changes that may reduce their risk of developing dementia, such as increasing physical exercise, stopping smoking and eating more healthily. Programmes like APPLE-Tree, which facilitate groups of adults with mild cognitive impairment to make changes through online support, are extremely valuable but access to these is currently limited. Coordinated investment and planning by the health, care and voluntary sectors to roll these programmes out more widely, targeting hard-to-reach communities in particular, is necessary for improving access to care.
“A common theme in dementia research is that the views of people with dementia and mild cognitive impairment are not always well-represented in service planning. To develop truly effective and accessible care, services must be designed alongside and jointly with service users and their families. A top down approach to dementia care may result in attractive headline outcomes, but may fail to deliver in terms of individual wellbeing.”
Sue Hilsdon - Carer and retired occupational therapist
“As a retired allied health professional (AHP) and carer for relatives with dementia, I have experienced the scenario on numerous occasions. Clinically (in AHP practice), people who were referred to our service for a variety of other presenting problems, are often found to have mild cognitive impairment or subjective cognitive decline. They are anxious about memory deficits, and we, as clinicians, are concerned as to the effectiveness, and longevity of the outcomes of our interventions. Additional information is always made available to support any memory loss. Certainly, in strength and balance classes it has been found that the activity and sociability of the group is valued by participants, and has an enduring effect on their well-being.
“As a carer, reassuring the person with memory problems becomes a regularly occurring task. It also becomes a situation where as a family member, there is heightened awareness, and a sense of impending doom! Promoting normal routines, patterns of behaviour and encouraging exercise and socialisation works but only in an environment where there are services/activities/facilities to support this. Reassurance (as a carer) that there is support available, is essential. 'Knowing the system', however, is an advantage in ensuring that timely and appropriate support is available.”
Most people caring for relatives with dementia experience loneliness
Read the Alert on loneliness in family caregivers
Peter Green - Former carer
“Until recently I was a carer for a family member with dementia, and I readily identify with feelings of loneliness. However, I suspect that in my case this was as much to do with the social restrictions imposed due to Covid-19 as caring for my relative. In normal times I would have met regularly with groups of friends and my children, and while I have kept in frequent contact via WhatsApp, FaceTime, etc, the lack of physical contact has been difficult. I imagine this must affect huge numbers of carers with limited social networks even more than it has me. If I had to do this again I would do my utmost to ensure I maintained my social contacts.
“This study is important in improving the understanding of causes of loneliness in carers and the impact this has on their health. It is relevant to those in a position to improve the wellbeing of carers, but it only suggests that action is required, without specifying what that might be.”
Dr Penny Rapaport - Clinical Psychologist
“This important research has helpfully explored the factors associated with experiencing loneliness. The authors found that carers were more likely to be lonely if they were socially isolated, felt stressed, had lower wellbeing themselves and had a poor-quality relationship with the person they cared for. During the Covid-19 pandemic, at a time where we are all experiencing barriers to social interaction, with complicated rules limiting our access to social support and our usual networks, this research feels particularly relevant.
“As a clinical psychologist and researcher working with family carers and people living with dementia, these findings fit with my experience that challenges in relationships and other factors that lead to feelings of loneliness have intensified for many over the past months. This research has reminded me that in any routine contact with family carers in health and social care settings, it is important to check in with them about how they are doing, talking with them about ways to connect with others and giving them space to say when things may not be going well. Services are also under pressure and resources limited, but these findings highlight that investing in social and psychological interventions for family carers that help them to overcome isolation and build connections are needed now more than ever.”
Ruth Hayes - Former carer
“As a former carer of a relative suffering from dementia, I am familiar with the need to learn quickly about the disease and how to navigate health and social care systems. The research suggests the Covid-19 pandemic has increased loneliness amongst carers for people with dementia with services for both the carer and cared for being restricted. It also points to the physical and mental health consequences of sustained loneliness.
“The research does not, however, discuss key practical problems associated with caring. For example, a loss of income arising through the need to reduce working hours adds to levels of stress and anxiety associated with caring, and further reduces carers’ abilities to participate in social and recreational activities. There is also the need to discover the language and procedures of social and health care providers who can support the person being cared for. Neither does the research address the stigma that is often attached to loneliness, nor the discomfort many carers feel when discussing their caring roles: too often they suffer in silence. This has implications for support providers who need to be highly sensitive and much more proactive when delivering services.
“The authors call for psychosocial interventions to reduce carer stress and improve the quality of the relationship between carers and people with dementia. Such approaches may well help, but providers should be armed with information on how carers can gain access to information on practical and financial support. Additionally the value of carer support groups as a means of reducing isolation and sharing information should be acknowledged.”
Ann Pascoe - Carer
“The Alert points out that carers can experience higher levels of loneliness if they have a poor-quality relationship with the person they care for. Rather than a poor-quality relationship, I think the level of loneliness can stem from the inability of the person with dementia to communicate or contribute to a diverse conversation with the carer. You can still have a caring and loving relationship but the conversation is often limited.
“The Covid-19 pandemic and lockdown has enabled me to get back to reading, studying and doing my own thing but it has also accentuated my role of being a carer rather than a wife. Being on call 24/7, every week, every month with no help has made me feel very alone rather than lonely. Throughout my involvement in carer activism I have never talked about loneliness but instead about being alone. Our family lives far away which has led them to give up on trying to help. It’s not an issue, as I understand where they’re coming from. Regarding dementia, however, I believe that you don’t have to fight it or beat it, you just have to accept it and get on with it.”
Occupational therapy at home may benefit people with dementia and their carers
Read the Alert on occupational therapy at home
Wendy Mitchell - Diagnosed with young onset dementia in 2014
“I’ve always found it strange that many other conditions, when diagnosed, have input from a qualified healthcare professional yet with dementia we rarely get offered help and support of this nature from the beginning and then as and when the need is there. Occupational therapists have so much to offer people with dementia as have many other professionals. This study shows the potential of what can be achieved from early intervention from a professional and I’m pleased and relieved to see that further research needs to be carried out to prove the cost-effective benefits.”
Working may improve quality of life for carers of people with dementia
Ann Pascoe - Carer
“I think that working can definitely improve your wellbeing as a carer and make you feel good. Working provides another stimulus and allows time away from caring which means that when you come home from work you’re able to devote quality time rather than quantity time. I reduced working after my stroke and have only done voluntary work during Covid which means I’m home all the time and without doubt have become a worse carer as a result. I now feel so guilty because my patience levels are near zero which means I can’t give Andrew the quality time that I used to. Although saying that, Andrew is actually happier because I’m here all the time but I still don’t feel that I’m giving him as much as I did before.
“I definitely believe that working outside the home leads to a better quality of life for the carer and I think that the Covid-19 pandemic has accentuated all of the issues surrounding caring.”
Peter Green - Former carer
“Anything which could help to improve the quality of life is to be welcomed, and it is hard to disagree with any of the results of this study. It is interesting to see the authors drawing an important distinction between quality of life and well-being. Sensibly, the paper steers clear of simplistic explanations, recognising the complexity of caring scenarios.
“Recognising that supporting carers to work outside the home is generally a good idea, but that there are negatives and practical difficulties, is one of the strengths of this study. Sadly, flexible working is not available to all, and the authors recognise that policy decisions may be required. I wonder how Covid-19 will influence the likelihood of this happening, as unemployment rates continue to rise. This Alert should be widely circulated.”
Loneliness, but not social isolation, predicts development of dementia in older people
Kathryn Walker - Clinical Research Nurse
“What is most thought provoking about this paper is that the results suggest that it is not necessarily the amount of social contact an individual has, but rather the quality of the social contact that can protect the ageing population from cognitive decline. This could have an interesting impact on the needs of patients requiring social care, using day centres and needing healthcare at home. Those without close relationships with family or friends would benefit from seeing the same carer/nurse/day centre staff and users at each visit; thus allowing them to form supportive friendships and develop a support structure to combat loneliness. Educating health and social care staff of this potential preventative measure would be beneficial both for the wellbeing of the patients, but also to the NHS as an achievable risk reduction measure against cognitive decline and associated clinical need.”
Training programme to improve communication between staff and patients with dementia in hospital shows promise
Read the Alert on the training programme
Emma Williams - Behaviour Analyst
“Communication between people with dementia and their carers is a recognised problem, which can cause distress and misunderstanding if handled inappropriately. This research and training programme has potential to be implemented in other areas, although further research is warranted. High staff turnover rates in places of care may be problematic to ensure people finish the course and implement the intervention successfully. The use of simple language has been documented to be successful in areas such as the provision of personal care, or engagement in activities. It is vital that we use evidence-based interventions to provide the best quality care to people with dementia.”
Ann Pascoe - Carer
“When Andrew was diagnosed with dementia I felt helpless. I realised that I knew nothing about the illness which is why I went back to university to do an MSc specifically in dementia. I have had to learn how to diffuse situations as opposed to arguing and have learned to walk away at the right moments. I’m really passionate about training and believe it has given me the wherewithal to deal with caring responsibilities.
“This research highlights a promising training programme that sounds fantastic but there seem to be concerns regarding costs. At Connecting Communities, we made the decision to put all of our training online not just because of lockdown but also due to the cost-effectiveness associated with online training compared to in-person training. To minimise costs and increase the accessibility of this particular training programme, I’m wondering why it can’t be done interactively online? The programme could then be shared with nurses, care home workers and even new carers. There is no doubt that training increases the confidence of carers and healthcare staff when communicating with people who have dementia. It can also ensure that the communication is done right more often than not.
“The presence of carers in hospitals can also really help improve the communication between staff and patients as they usually have a better understanding of the person with dementia. Incorporation of dementia training in nursing degrees which has input from carers and people with dementia is also crucial. For the past five years this has provided nursing students at Scottish universities with a really good grounding in dementia.”
Kathryn Walker - Clinical Research Nurse
“As reported in this paper, up to 25% of acute hospital beds are used by patients with a diagnosis of dementia. This is a huge population of people that would benefit from adjusted communication methods to make their hospital stay an easier experience for both them and the healthcare staff caring for them. Admission to hospital is often a massive upheaval for patients living with dementia. At home, these individuals have their own routine, their own coping strategies, to keep life as regular and as manageable as possible. Once in hospital, the ward routine takes over and difficulties can occur due to the unfamiliar environment, fast and complex communication in a very busy clinical setting, and alterations to the patients daily schedule. This study suggests that the provision of staff communication training for patients living with dementia would be extremely beneficial, providing more patient-centred care for this patient group and making their hospital stay a more pleasant and bearable experience.”
Isobel Chick - Speech and Language Therapist
“Multiple barriers to effective care exist for people with dementia. Barriers include aphasia (difficulty understanding and using language), ethnicity, frequent staff turnover and lack of early specialist support for people with mild cognitive impairment (‘pre-dementia’). Barriers such as these can lead to social isolation and loneliness, exacerbating changes to cognition and memory and resulting in diminished quality of life.
“Aphasia is a particular concern. As dementia progresses, occasional word-finding difficulties often progress to pervasive impairments in understanding and using spoken language and non-verbal communication, such as gestures and facial expressions. Communication difficulties, on top of stressors such as hospital admissions or separation from family, can result in significant confusion and distress. Targeted training programmes which support care staff to understand aphasia and adapt how they communicate with people with dementia, provide a pathway to more effective care.”
A less healthy lifestyle increases the risk of dementia
Tom Russ - Consultant Psychiatrist
“This adds to the well-established evidence that multiple lifestyle factors throughout the life course influence one's risk of developing dementia. The 2020 Lancet Commission provides a broader view but all the published reports conclude that approximately a third of dementia risk relates to potentially modifiable lifestyle factors.”
Goal-setting can help people with early-stage dementia improve function

Read the Alert on goal-setting
Wendy Mitchell - Diagnosed with young onset dementia in 2014
“An interesting study with a surprising outcome for me. How do you measure quality of life as compared to what? Continuing to hold onto any independence and skill is so important for people with dementia as the condition itself strips away so much from our everyday life. I wondered if the cost was due to occupational therapists being the people who delivered the intervention? It would have been cheaper for a Dementia Support Worker maybe to deliver. I think this study had a valuable goal but perhaps needs to be approached from a different angle and quality of life measure to be re-designed.”
Dementia Care Mapping: Care home managers and staff need more support to improve care
Read the Alert on Dementia Care Mapping
Isobel Chick - Speech and Language Therapist
“Staff turnover, in hospitals and in the community, is clearly a barrier to effective care for people with dementia. Interventions such as Dementia Care Mapping (DCM), which is designed to support care home staff understand life from the perspective of a person with dementia, have the potential to significantly increase staff awareness of dementia and improve care. However, the effectiveness of DCM and other similar programmes rely on stable and consistent staffing. Care managers need support in the practicalities of running these programmes; for example, how to manage competing priorities and staff absences, and integrate new staff effectively? DCM and other programmes must be designed to operate within the current realities of the care sector: care homes lack staff and turnover is common. Reducing turnover and upskilling staff must be a key priority in improving care.”
Join Dementia Research
If you would like to help advance dementia diagnosis, care and treatment, you can sign up to Join Dementia Research. By registering your details on the service, you are matched to various studies across the UK . When this happens, researchers will be in touch to see if you want to take part.
You don’t need to have a dementia diagnosis to take part - we also need healthy volunteers in order to gain a better understanding of how dementia develops.
You can either sign up via the website or by calling one of our charity partner helplines.
Learn more about our contributors
Penny is a Clinical Psychologist and Research Fellow in the Division of Psychiatry at UCL. Having worked for a number of years in services for older people in the NHS she is interested in developing deliverable and sustainable psychosocial interventions. Her research interests include collaborating on the development, testing and implementation of non-pharmacological interventions for people living with dementia, their families and paid carers.
Peter is a member of the public who until recently was an unpaid carer for an elderly relative with dementia and several other ailments. He also has another relative recently diagnosed with Alzheimer's disease. As a result, Peter is very aware of the toll caring can take on people. He worked in the NHS in a non-medical role for 30 years and continues to have an interest in science and medicine.
Ann’s husband was diagnosed with Vascular Dementia in 2006. By 2010 she was a carer activist, setting up the first Scottish rural Dementia Friendly Community in 2012. Ann completed an MSc (Dementia) at Stirling University and later joined the NHS Highland Board before becoming a carer statistic in 2017 when she had a stroke.
Mohammed Akhlak Rauf MBE is the founder and director of Meri Yaadain Community interest Company (CiC). He has over 25 years experience of working with BAME communities and on health inequalities. Akhlak has also spent 15 years working with BAME people living with or caring for a relative with dementia.
Isobel is a Speech and Language Therapist working in the community with adults with speech, language, communication and swallowing difficulties due to neurological conditions such as stroke, dementia and Parkinson’s. She is particularly interested in advances in aphasia therapy and changes in language processing across the lifespan, including healthy ageing.
Wendy was diagnosed with young onset dementia in 2014. “So often the diagnosis process can feel a very negative experience concentrating on our failures and offering no hope. If only it was normal for clinicians to talk about research in a positive way at every opportunity then at least it would give us that chink of hope we so desperately need.”
Sue is a retired Community Occupational Therapist and carer for relatives with dementia. She has experienced many of the situations discussed within the Alerts on numerous occasions, in her professional and personal life.
Emma is a Board Certified Behaviour Analyst, experienced in working with people who have dementia in both private and NHS settings. Emma is a current PhD student at Bangor University, specialising in behaviour analytic research in diverse areas.
Kathryn Walker is a Clinical Research Nurse at Newcastle NIHR Clinical Ageing Research Unit, a collaborative clinical research department affiliated with both the Newcastle upon Tyne Hospitals NHS Foundation Trust and Newcastle University. Kathryn specialises in coordinating clinical trials in conditions linked to the ageing population; in particular movement disorders and different forms of dementia.
Tom Russ is a Consultant Psychiatrist and Director of the Alzheimer Scotland Dementia Research Centre at the University of Edinburgh.
Ruth is a social researcher specialising in health and social care. She is also a former carer for a relative who suffered with dementia and has experience of caring for a spouse who was successfully treated for cancer
NIHR Evidence is covered by the creative commons, CC-BY licence. Written content and infographics may be freely reproduced provided that suitable acknowledgement is made. Note, this licence excludes comments and images made by third parties, audiovisual content, and linked content on other websites.











 Dr Penny Rapaport
Dr Penny Rapaport Peter Green
Peter Green Ann Pascoe
Ann Pascoe Mohammed Akhlak Rauf MBE
Mohammed Akhlak Rauf MBE Isobel Chick
Isobel Chick  Wendy Mitchell
Wendy Mitchell Sue Hilsdon
Sue Hilsdon Emma Williams
Emma Williams Kathryn Walker
Kathryn Walker Tom Russ
Tom Russ Ruth Hayes
Ruth Hayes